Laparoscopic Removal of Paraovarian Cyst and Appendix: Advances in Minimally Invasive Surgery
Add to
Share
3,257 views
Report
1 year ago
Description
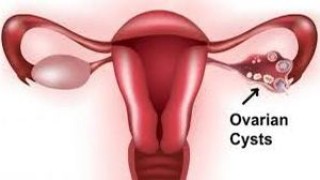
Laparoscopic Removal of Ovarian Cyst and Appendix: Advances in Minimally Invasive Surgery Introduction Minimally invasive surgery has revolutionized the field of medicine by offering procedures that minimize patient discomfort and hasten recovery times. Among these procedures, laparoscopic removal of ovarian cysts and appendectomy stand out due to their effectiveness and efficiency. This article discusses the techniques, benefits, and considerations of performing laparoscopic surgeries for ovarian cysts and the appendix. Laparoscopic Surgery for Ovarian Cysts Ovarian cysts are fluid-filled sacs that develop on the ovaries and are often benign. However, they can sometimes grow large, rupture, or cause pain, necessitating surgical intervention. Laparoscopy, also known as keyhole surgery, is frequently employed to remove these cysts with minimal disruption to the patient's life. During the procedure, a small incision is made in the navel through which a laparoscope (a long, thin tube with a high-intensity light and a high-resolution camera at the front) is inserted. Additional small incisions are made for instruments that allow the surgeon to access and remove the cyst. The benefits of this approach include reduced post-operative pain, minimal scarring, and a quicker return to daily activities. Laparoscopic Appendectomy Appendectomy, the surgical removal of the appendix, is typically performed as an emergency procedure in the case of appendicitis. Laparoscopic appendectomy involves several small incisions in the abdomen through which surgical tools and a camera are inserted to remove the appendix. The clear visualization provided by the laparoscope allows for precise removal, reducing the risk of complications. This technique is particularly advantageous for obese patients and those with a complicated appendicitis, as it reduces the risk of wound infections and postoperative hernias. Moreover, the recovery period is shorter compared to traditional open surgery. Technical Considerations The success of laparoscopic surgery for ovarian cysts and appendectomy largely depends on the surgeon’s skill and the complexity of the case. Surgeons must be proficient in manipulating instruments within limited visibility and space. Furthermore, the decision to opt for laparoscopy over traditional methods should consider patient-specific factors such as previous abdominal surgery, which might increase the risk of adhesions. Recovery and Postoperative Care Postoperative care is crucial for a smooth recovery. Patients are generally advised to follow a specific diet, avoid strenuous activities, and watch for signs of infection around the incision sites. Most patients can resume normal activities within a week, although complete recovery may take slightly longer. Conclusion The laparoscopic removal of ovarian cysts and the appendix represents significant advancements in the field of minimally invasive surgery. With benefits such as reduced pain, shorter hospital stays, and quicker recovery times, these procedures exemplify the progress in surgical technologies aimed at enhancing patient outcomes. As techniques continue to evolve, the scope of laparoscopic surgery is likely to expand, offering patients safer and more effective treatment options. References Society of American Gastrointestinal and Endoscopic Surgeons (SAGES) American College of Surgeons This article aims to inform both healthcare professionals and patients about the potential and advantages of laparoscopic procedures in treating common conditions like ovarian cysts and appendicitis, highlighting the importance of technological integration in surgical practices. A paraovarian cyst, also known as a paratubal cyst, is a type of cyst that forms in the adnexa of the uterus, which includes the ovaries, fallopian tubes, and surrounding tissues. These cysts are typically benign (non-cancerous) and arise from the epithelial remnants of the Wolffian duct (also known as the mesonephric duct), which are sometimes left behind during the embryonic development of the female reproductive tract. Here are some key points about paraovarian cysts: Location and Composition: Paraovarian cysts are located next to the ovary but are not actually part of the ovarian tissue. They are most often filled with clear fluid and are encased in a thin wall. Symptoms: In many cases, paraovarian cysts are asymptomatic and are discovered incidentally during pelvic examinations or imaging studies for other reasons. However, if they grow large, they can cause pelvic pain, discomfort, or bloating. Large cysts may also exert pressure on other pelvic organs. Diagnosis: These cysts are typically diagnosed through imaging techniques such as ultrasound, CT scan, or MRI. On ultrasound, they appear as clear, fluid-filled sacs located adjacent to the ovaries. Management: The management of paraovarian cysts depends on their size and the symptoms they produce. Small, asymptomatic cysts may be monitored over time with periodic ultrasounds. If a cyst is large or causing symptoms, surgical removal might be recommended. This is usually done laparoscopically, which is a minimally invasive surgical approach. Risks and Complications: While generally benign, paraovarian cysts can cause complications such as torsion (twisting), rupture, or infection, although these are relatively rare. Understanding the nature of paraovarian cysts is important for appropriate management and treatment, particularly in distinguishing them from ovarian cysts, which can have different implications and treatment pathways.
Similar Videos