Laparoscopic Management of Ectopic Pregnancy: An Overview
Add to
Share
3,483 views
Report
1 year ago
Description
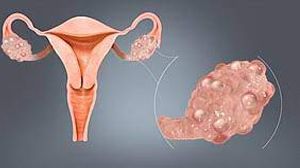
Introduction Ectopic pregnancy, a condition where a fertilized egg implants outside the uterine cavity, often in the fallopian tube, poses significant health risks to women of reproductive age. It is a leading cause of pregnancy-related morbidity and mortality in the first trimester. Early diagnosis and management are crucial. Laparoscopic surgery has emerged as the gold standard for treating ectopic pregnancies due to its minimally invasive nature, reduced recovery times, and lower complication rates compared to traditional open surgery. Diagnosis Early diagnosis of ectopic pregnancy relies on a combination of clinical assessment, transvaginal ultrasound, and serial measurement of serum beta-hCG (human chorionic gonadotropin) levels. Common clinical signs include pelvic pain, vaginal bleeding, and a positive pregnancy test. Ultrasound typically reveals the absence of an intrauterine gestational sac and may identify an adnexal mass or free pelvic fluid. Indications for Laparoscopic Surgery Laparoscopic management is indicated in most cases of ectopic pregnancy, especially when the patient is hemodynamically stable and there is no evidence of significant intra-abdominal bleeding. Indications include: Unruptured ectopic pregnancy Hemodynamically stable patient Desire for future fertility Failed medical management with methotrexate Surgical Technique Laparoscopic management of ectopic pregnancy involves several key steps: Preparation and Anesthesia: The patient is placed under general anesthesia. Preoperative preparations include ensuring appropriate hemoglobin levels and availability of blood products in case of emergency. Trocar Placement: Typically, a three-port technique is used. A 10-mm trocar is inserted at the umbilicus for the laparoscope, and two 5-mm trocars are placed in the lower abdomen for surgical instruments. Inspection and Diagnosis: The pelvic cavity is inspected to confirm the diagnosis. The ectopic pregnancy is usually located in the fallopian tube, but other locations like the ovary or abdominal cavity should be considered. Salpingectomy or Salpingostomy: Salpingectomy: If the fallopian tube is severely damaged or there is significant bleeding, the affected segment of the tube is removed. This involves coagulating and cutting the mesosalpinx and the tubal segments. Salpingostomy: For patients desiring future fertility and when the tube is relatively undamaged, a linear incision is made on the antimesenteric border of the tube. The ectopic pregnancy is carefully removed, and the tubal incision is left to heal by secondary intention. Hemostasis and Closure: Hemostasis is achieved using bipolar cautery or sutures. The abdominal cavity is irrigated to remove blood and debris. Ports are then removed, and the incisions are closed with sutures or skin adhesive. Postoperative Care Postoperative care involves monitoring for complications such as bleeding, infection, and persistent trophoblastic tissue. Serial beta-hCG levels are measured to ensure complete resolution of the ectopic pregnancy. Patients are advised to avoid pregnancy for at least three months to allow for complete recovery and tubal healing. Advantages of Laparoscopic Management Laparoscopic surgery offers several advantages over open surgery, including: Reduced postoperative pain Shorter hospital stay Faster recovery and return to normal activities Lower risk of adhesions and subsequent infertility Improved cosmetic outcomes Complications and Considerations While laparoscopic management is generally safe, potential complications include: Intraoperative bleeding Damage to surrounding organs (e.g., bowel, bladder) Incomplete removal of ectopic tissue Conversion to open surgery in case of complications Conclusion Laparoscopic management of ectopic pregnancy is a highly effective and safe approach, providing numerous benefits over traditional open surgery. With advances in laparoscopic techniques and equipment, most ectopic pregnancies can be managed with minimal invasiveness, ensuring better outcomes for patients. Early diagnosis and timely intervention remain critical to reduce the morbidity and mortality associated with this condition.
Similar Videos