Minimally Invasive Approach to Correcting Complete Indirect Inguinoscrotal Hernia
Add to
Share
1,741 views
Report
1 year ago
Description
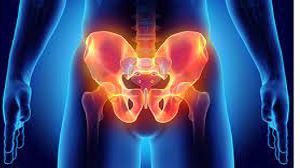
Minimally Invasive Approach to Correcting Complete Indirect Inguinoscrotal Hernia: A Laparoscopic Solution Introduction Indirect inguinoscrotal hernias, characterized by the protrusion of abdominal contents through the inguinal canal into the scrotum, present significant challenges for surgical correction. Traditional open repair methods, while effective, often come with extended recovery times and increased post-operative discomfort. Advances in minimally invasive surgical techniques, particularly laparoscopic surgery, have revolutionized the management of these hernias, offering patients a safer, less painful alternative with quicker recovery times. Understanding Indirect Inguinoscrotal Hernias Indirect inguinoscrotal hernias occur when the hernia sac follows the path of the inguinal canal, potentially extending into the scrotum. This type of hernia is more common in males due to the anatomical structure of the inguinal region. Patients typically present with a visible or palpable bulge in the groin or scrotum, discomfort, and sometimes pain, especially when lifting or straining. The Laparoscopic Solution Laparoscopic surgery, a form of minimally invasive surgery, involves the use of small incisions, a camera, and specialized instruments to repair the hernia. This approach contrasts sharply with the larger incisions required for open surgery, resulting in several significant benefits. Advantages of Laparoscopic Repair 1. Reduced Post-operative Pain: Smaller incisions mean less tissue damage and consequently less pain after surgery. 2. Shorter Recovery Time: Patients can return to their daily activities and work more quickly compared to those who undergo open surgery. 3. Lower Risk of Infection: The smaller incisions reduce the exposure of internal tissues to potential contaminants, lowering the risk of post-operative infections. 4. Better Cosmetic Outcomes: The smaller scars are less noticeable than the larger scars left by open surgery. Procedure Overview The laparoscopic repair of an indirect inguinoscrotal hernia involves several key steps: 1. Anesthesia: The procedure is typically performed under general anesthesia. 2. Incision and Access: Three small incisions are made—one for the laparoscope (a small camera) and two for the surgical instruments. 3. Hernia Sac Identification: The hernia sac is identified, and the protruding contents are gently pushed back into the abdominal cavity. 4. Mesh Placement: A synthetic mesh is placed over the defect in the abdominal wall to strengthen the area and prevent recurrence. 5. Closure: The incisions are closed with sutures or surgical glue. Case Studies and Outcomes Numerous studies have demonstrated the effectiveness of laparoscopic hernia repair. For example, a study involving 500 patients showed a recurrence rate of less than 2%, with most patients reporting minimal pain and a high satisfaction rate post-surgery. Another study highlighted that laparoscopic repair reduced hospital stay durations significantly compared to open surgery. Conclusion Laparoscopic repair of complete indirect inguinoscrotal hernias offers a minimally invasive, effective solution with numerous advantages over traditional open surgery. Patients benefit from reduced pain, quicker recovery, and lower infection rates, making it an increasingly preferred option for both surgeons and patients. As surgical techniques and technologies continue to evolve, the success rates and benefits of laparoscopic hernia repair are likely to improve even further, solidifying its role as a standard treatment for inguinoscrotal hernias.
Similar Videos